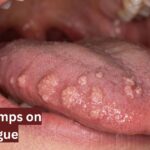
HPV bumps on tongue are small, painless growths caused by the human papillomavirus. These bumps can appear on the tongue, lips, and inner mouth. Many people do not notice them at first. HPV bumps on tongue are more common than most people think. They can spread if left untreated. Early detection makes treatment much easier.
HPV bumps on tongue come in different types. Each type looks and behaves differently. Some are soft and cauliflower-shaped. Others are rough and thick. A weak immune system increases the risk of getting them. Poor oral hygiene and tobacco use also raise the chances. Knowing the causes, types, and treatment options helps you take the right action fast. This guide covers everything you need to know about HPV bumps on tongue in simple, clear terms.
Related Post: Red circle on skin not ringworm? Here’s when to visit the ER of Irving
What Does Oral HPV Look Like?
Oral HPV does not always announce itself clearly. Many people carry the virus for months or even years without visible symptoms. However, when HPV does produce oral lesions, certain visual patterns tend to repeat.
Common characteristics of oral HPV bumps include:
- Small, raised or flat growths on the tongue, inner cheeks, or soft palate
- Clusters of bumps rather than single, isolated spots
- White, pink, or flesh-colored appearance
- Soft or slightly rough texture depending on the HPV strain involved
- Bumps on the back of the tongue, lip line, or near the throat
- Lesions that do not cause pain but may cause mild discomfort when eating or swallowing
It is worth noting that oral HPV bumps do not look the same in every case. Their appearance varies based on which specific HPV strain is responsible, where exactly the lesion forms, and the overall health of the individual’s immune system.
If you notice any new or unusual growth inside your mouth that does not resolve within two weeks, seeking professional evaluation is strongly advised.
HPV Types
More than 200 strains of human papillomavirus have been identified, and around 40 of these are associated with oral warts and lesions. Each strain behaves differently, produces a distinct type of growth, and requires a tailored approach to treatment. Knowing the specific type of HPV bump you may be dealing with is a critical first step toward effective care.
Squamous Papilloma
Squamous papilloma is the most frequently diagnosed oral HPV lesion. It is typically caused by HPV strains 6 and 11 and presents as a small, soft, cauliflower-like growth that measures less than 1 cm in diameter. The surface is covered with tiny finger-like projections, giving it a distinctive texture. The color ranges from white to pinkish-red.
These growths commonly appear on the tongue, palate, gums, tonsils, and inner cheeks. They are generally benign and rarely become cancerous. Most people discover them during routine dental checkups because they produce no pain or noticeable discomfort.
Verruca Vulgaris
Also known as the common wart, Verruca vulgaris is most often found on the skin of the hands and feet, but it can also develop inside the oral cavity particularly on the lips, inner cheeks, and tongue. It is caused by HPV strains 2 and 4 and accounts for roughly 70% of all wart infections.
Unlike squamous papilloma, verruca vulgaris has a rougher, thicker surface. The growth is well-defined, typically under 1 cm, and may appear white or slightly pink. In the mouth, it can cause mild irritation when it comes into contact with teeth or dental appliances.
Condyloma Acuminatum
Condyloma acuminatum commonly called a venereal wart is strongly associated with sexual transmission, particularly oral-genital contact. It is caused by HPV strains 2, 6, and 11. These lesions tend to be larger than squamous papillomas, often appearing in multiple clusters, and are soft and pink with a wart-like, cauliflower-shaped surface.
In the oral cavity, condyloma acuminatum most often develops on the tongue, inner lips, and soft palate. Because of its strong link to sexual activity, its presence may also indicate other sexually transmitted infections, and comprehensive STI screening is recommended.
Focal Epithelial Hyperplasia
Focal epithelial hyperplasia, also known as Heck’s disease, is a rare form of oral HPV caused by strains 13 and 32. It typically presents as multiple, soft, flattened or rounded nodules scattered across the inner cheeks, lips, and tongue. Unlike the other HPV types, Heck’s disease is not associated with sexual transmission it spreads primarily through close personal contact and is more commonly seen in children and certain ethnic populations.
The lesions are usually painless, flesh-colored, and do not bleed. Because they are so flat, they can sometimes be overlooked during routine examination.
HPV vs. Herpes: Know the Difference
HPV and herpes (HSV) are both viral infections that can affect the mouth and lips, and they are frequently confused with one another. However, they are caused by entirely different viruses and behave in very distinct ways.
| Feature | HPV (Human Papillomavirus) | Herpes (Herpes Simplex Virus) |
| Virus Type | Human papillomavirus (HPV) | Herpes simplex virus (HSV-1 or HSV-2) |
| Appearance | Small, raised, firm wart-like bumps | Fluid-filled blisters that rupture and crust |
| Pain Level | Usually painless or mildly uncomfortable | Often painful, with burning or tingling before outbreak |
| Location in Mouth | Tongue, inner cheeks, soft palate, lips | Lips, gum line, roof of mouth (HSV-1) |
| Outbreak Pattern | Persistent growths, do not come and go | Recurrent flare-ups triggered by stress or illness |
| Healing | May persist for months without treatment | Blisters heal within 1–2 weeks on their own |
| Cancer Risk | Some high-risk strains are linked to oral cancer | Not associated with cancer |
The key distinction is that HPV bumps are typically firm, wart-like, and painless, while herpes sores appear as fluid-filled blisters that cause burning, itching, or tingling before they emerge. When in doubt, a clinical evaluation and lab testing are the only reliable ways to confirm a diagnosis.
How Is Oral HPV Caused?
Oral HPV is transmitted when the virus enters the body through broken or damaged tissue in the mouth or throat. It does not require an open wound microscopic abrasions that occur naturally during daily activities can be sufficient for the virus to take hold.
The most common causes and risk factors for oral HPV include:
- Oral sexual contact oral-genital contact is the primary transmission route for most oral HPV infections
- Mouth-to-mouth contact deep kissing can transfer HPV particles through saliva and mucus
- Multiple sexual partners having more than one sexual partner significantly raises the risk of exposure
- Shared utensils or personal items using contaminated forks, spoons, lip balm, or toothbrushes can facilitate transmission
- Weakened immune system individuals with compromised immunity are far more likely to develop visible symptoms
- Tobacco and alcohol use regular use damages oral tissues, making them more susceptible to HPV infection
- No HPV vaccination unvaccinated individuals have a higher risk of contracting strains covered by available vaccines
- Poor oral hygiene bacteria and inflammation create an environment where the virus can more easily establish itself
It is important to note that not everyone who contracts HPV will develop visible bumps. In many cases, a healthy immune system clears the infection before it ever produces symptoms.
Can HPV Bumps on the Lips Spread?
Yes because HPV is a viral infection, it is contagious and can spread both to other areas of the body and to other people.
HPV bumps on the lips are considered especially contagious when active, meaning they are visible and developing. The virus can migrate from the lip line to the inner mouth, tongue, cheeks, soft palate, and even the throat. Physical contact with an active lesion whether through kissing, oral sex, or even touching the bump and then touching another part of the mouth can transmit the virus.
White bumps appearing on the lip line are a visible sign that the virus is active and spreading. At this stage, close personal contact should be limited and medical evaluation sought promptly.
Within the oral cavity itself, HPV most commonly spreads to:
- The front and back of the tongue
- The inner cheeks and floor of the mouth
- The soft palate
- The tonsils and throat
Persistent or spreading oral HPV warrants professional assessment, not only for treatment but also to rule out any progression toward oropharyngeal cancer HPV is responsible for approximately 70% of cancers of the throat, tonsils, and base of the tongue.
HPV Bumps Treatment
There is currently no cure for HPV itself, but the bumps and lesions it produces can be effectively treated through a range of medical and natural approaches. The right treatment depends on the type of HPV involved, the size and location of the lesion, and the overall health of the patient.
Medical Treatment Options
Surgery
Surgical excision is one of the most direct methods for removing HPV bumps that are large, persistent, or resistant to other treatments. The procedure is typically performed by a dentist, ENT specialist, or oral surgeon under local anesthesia. The growth is physically cut away using a scalpel or specialized surgical instrument. Recovery is generally quick, and the removed tissue can be sent for biopsy to rule out malignancy.
Therapies
Cryotherapy uses liquid nitrogen to freeze HPV lesions at extremely low temperatures, causing the tissue to die and the bump to fall off naturally within a week or two. It is considered one of the most effective removal methods and works particularly well for HPV bumps on the lips and accessible areas of the oral cavity. Multiple sessions may be required for larger or more stubborn lesions.
Laser therapy uses focused light energy to precisely destroy HPV-infected tissue with minimal damage to surrounding healthy tissue. It is the preferred option for hard-to-reach growths such as lesions at the back of the tongue or deep in the throat because of the precision and control it offers. Laser therapy also carries a lower risk of scarring and post-procedure bleeding compared to surgical excision.
Medications
Topical medications in the form of prescription creams and gels can be applied directly to accessible HPV lesions. Imiquimod, an immune-enhancing cream, stimulates the body’s own immune response to attack the infected tissue. Research has shown it to be effective and well-tolerated even in oral applications. Trichloroacetic acid (TCA) is another option, which works by causing chemical coagulation of the wart tissue and is particularly useful for widespread lesions. These medications are generally prescribed by a physician and are more suitable for external or easily accessible bumps.
Electrosurgery
Electrosurgery uses a controlled electrical current to burn off HPV-infected tissue. The procedure is typically fast and performed under local anesthesia for smaller lesions, or general anesthesia when multiple or large lesions are involved. While effective, electrosurgery does carry some risk of scarring and post-procedure discomfort. It is generally recommended when other approaches are not practical or when a tissue sample is required for pathological examination.
Natural Way of Healing
While natural approaches cannot eliminate HPV from the body, they can support the immune system’s ability to suppress the virus and may help reduce the frequency and severity of outbreaks.
Improving the Immune System
A robust immune system is the body’s best defense against HPV. Many oral HPV infections clear on their own when the immune system is functioning well. Supporting immune health includes:
- Eating a diet rich in fruits, vegetables, and whole grains
- Getting regular, moderate exercise
- Prioritizing sleep and managing chronic stress
- Considering immune-supportive nutrients such as vitamin C, zinc, and folate under medical guidance
Avoiding Harmful Products
Tobacco and alcohol are two of the most significant lifestyle factors that worsen HPV outcomes. Both damage the mucosal lining of the mouth, reduce immune response, and create conditions that allow the virus to thrive. Eliminating tobacco use and reducing alcohol consumption are meaningful steps that support both treatment and prevention.
Better Oral Hygiene
Maintaining excellent oral hygiene reduces the bacterial load in the mouth, limits inflammation, and creates a less hospitable environment for the virus. This includes brushing twice daily with a fluoride toothpaste, flossing regularly, using an antimicrobial mouthwash, and keeping up with routine dental checkups. Early detection during dental visits is one of the most reliable ways to catch oral HPV lesions before they progress.
Conclusion
HPV Bumps on Tongue are more common than many people expect and more manageable than many fear. The key is recognizing them early, understanding which type of HPV may be involved, and choosing the right treatment approach based on the severity and location of the lesion.
Whether you opt for a clinical procedure like cryotherapy or laser removal, or you focus on strengthening your immune system through lifestyle changes, taking action promptly makes a significant difference in outcomes. HPV bumps that are caught and addressed early are far less likely to persist, spread, or develop into something more serious.
If you notice any new, unusual, or persistent growth in your mouth, do not wait. A professional evaluation is the only way to get an accurate diagnosis and the first step toward effective treatment.
FAQs
What are the early symptoms of oral HPV?
The earliest signs are usually small, raised or flat painless bumps on the tongue, inner cheeks, or soft palate that do not heal on their own within two weeks.
How do you spot the difference between a normal bump and an HPV bump?
Normal mouth bumps such as canker sores or minor irritations typically resolve within 7 to 14 days on their own, whereas HPV bumps persist, may grow, and often appear in clusters rather than in isolation.
How can you kill HPV naturally?
While there is no proven natural cure, a strong immune system can suppress the virus; eating well, exercising regularly, avoiding tobacco and alcohol, and maintaining good oral hygiene all support the body’s ability to clear HPV on its own.
Can oral HPV turn into cancer?
Yes, certain high-risk HPV strains particularly HPV-16 have been strongly linked to oropharyngeal cancers of the tongue, tonsils, and throat, which is why persistent oral lesions should always be evaluated by a healthcare professional.
Is there a vaccine for oral HPV?
Yes, the HPV vaccine (Gardasil 9) is highly effective at preventing infection from the most common high-risk and low-risk strains, and is recommended for adolescents and young adults up to age 26, and in some cases up to age 45 following medical consultation.