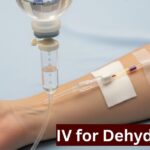
Dehydration can turn dangerous faster than most people expect. One moment you feel a little tired and thirsty. The next, you’re dizzy, confused, and unable to keep a sip of water down. When your body loses fluids faster than you can replace them, drinking water simply isn’t enough and that’s exactly when an IV for dehydration becomes a life-saving intervention.
Related Post: Recognizing the Signs of Dehydration: A Complete Guide
What Is IV Hydration?
At ER of Irving, our emergency team treats dehydration every single day. Whether it’s a child burning up with fever, an adult laid flat by food poisoning, or a patient recovering from heat exhaustion, intravenous (IV) hydration is often the fastest, most reliable path to recovery. This guide covers everything you need to know from recognizing the signs to understanding which IV fluids are used and what to expect at the ER.
IV hydration is a medical treatment that delivers a sterile solution of fluids, electrolytes, and sometimes glucose directly into your bloodstream through a thin catheter placed in a vein typically in your arm or hand.
Unlike drinking water or sports drinks, which must pass through your digestive system before your body absorbs them, IV fluids bypass that process entirely. The result is near-immediate rehydration. As one medical expert noted, it can take up to an hour for your body to process a liter of water through the stomach, whereas an IV delivers fluid directly into the vein right away.
IV hydration isn’t just for hospitals. Urgent care centers and emergency rooms both administer IV fluids for patients who need faster rehydration than oral intake can provide.
When Do I Need an IV for Dehydration?
Not every case of dehydration requires an IV. Mild dehydration where you feel thirsty and a little fatigued typically responds well to drinking water or an oral rehydration solution. But moderate to severe dehydration is a different story.
You may need an IV for dehydration if you:
- Cannot keep any fluids down due to persistent vomiting or diarrhea
- Feel faint, lightheaded, or have actually passed out
- Have a rapid or irregular heartbeat
- Show signs of confusion, disorientation, or extreme weakness
- Notice dark amber urine, or haven’t urinated in several hours
- Are a young child or infant who is visibly lethargic or has no tears when crying
- Are an older adult with underlying conditions like kidney disease or diabetes
These are warning signs that your body is struggling to maintain normal function. IV hydration at this stage isn’t optional it’s urgent.
How to Tell If You Need an IV for Dehydration
One of the most reliable self-checks for dehydration is the skin turgor test: pinch the skin on the back of your hand or forearm. In a well-hydrated person, the skin snaps back immediately. If it stays “tented” slow to return to flat you’re likely significantly dehydrated.
Other reliable indicators include:
- Urine color: Pale yellow is healthy. Dark amber or brown means your kidneys are conserving water a red flag.
- Urination frequency: If you haven’t needed the bathroom in 8+ hours, that’s a serious sign.
- Mental clarity: Confusion, brain fog, or slurred speech alongside thirst requires immediate evaluation.
- Dry mouth and sunken eyes: Common in moderate-to-severe cases, especially in children.
At ER of Irving, our team doesn’t guess. We run on-site lab tests to check your electrolyte levels, blood chemistry, and kidney function giving us a precise picture of your hydration status within minutes.
What IV Is Given for Dehydration? The 4 Main Types
The right IV fluid depends on your specific condition, the cause of your dehydration, and your electrolyte levels. Healthcare providers choose from four primary options:
| IV Fluid | Composition | Best Used For |
| Normal Saline (0.9% NaCl) | Sterile water + sodium chloride | General dehydration, most common first-line fluid |
| Lactated Ringer’s (LR) | Sodium, potassium, calcium, lactate | Trauma, severe illness, cardiac cases, complex dehydration |
| Dextrose 5% in Water (D5W) | Water + 5% glucose | Prolonged dehydration, low blood sugar, energy restoration |
| Half Normal Saline (0.45% NaCl) | Lower concentration salt solution | Mild dehydration, hypernatremia correction, specific clinical needs |
Normal Saline
The most widely used IV fluid in emergency settings. It’s an isotonic solution meaning it matches your blood’s osmotic pressure making it safe for most patients. It replenishes blood volume quickly and is the standard starting point for general dehydration treatment.
Lactated Ringer’s Solution
Lactated Ringer’s is considered more physiologically balanced than normal saline. It contains a combination of electrolytes that closely mimic blood plasma, which makes it the preferred choice for trauma patients, those with severe GI losses, and complex cardiac cases. Some research suggests it may be better for preventing metabolic acidosis compared to large-volume normal saline infusions.
Dextrose 5% in Water (D5W)
D5W provides both fluid and a quick energy source. It’s typically used when a patient has been dehydrated for an extended period and their blood glucose is low. It’s also used in specific metabolic conditions where a pure saline solution isn’t appropriate.
Half Normal Saline (0.45% NaCl)
A hypotonic solution used for milder dehydration or cases involving high sodium levels (hypernatremia). Because it has a lower salt concentration, it’s used selectively and always under close medical supervision.
Important: Only a licensed healthcare provider can determine which IV fluid is right for your condition. Never attempt to self-administer IV fluids outside a medical setting.
How Long Does IV Hydration Last?
An IV hydration session at ER of Irving typically takes 30 to 60 minutes, though this varies based on the severity of your dehydration and which fluid is being administered. Severe cases may require a longer infusion or multiple bags.
Once the IV is complete, most patients feel a noticeable improvement better energy, reduced dizziness, and clearer thinking that can last 1 to 2 days. However, the goal isn’t just short-term relief. Our team monitors your vitals throughout and provides discharge instructions to prevent relapse, including oral hydration targets and follow-up care recommendations.
IV Fluids for Dehydration: How Many Bags?
The number of IV fluid bags you receive depends on your level of dehydration and your body’s response to treatment:
- Mild to moderate dehydration: 1 bag (500–1,000 mL) is usually sufficient to restore fluid balance and stabilize symptoms.
- Severe dehydration: 2 to 3 bags may be needed, particularly in cases involving prolonged vomiting, diarrhea, or heatstroke.
- Complex cases (e.g., kidney issues, electrolyte imbalances, or co-existing illness): The provider will adjust volume based on real-time lab results and clinical response.
There’s no universal answer your ER physician determines the right amount during your visit.
Common Conditions That Cause Dehydration
Dehydration rarely happens in isolation. It’s almost always triggered by an underlying condition or circumstance. The most common causes we treat at ER of Irving include:
- Food poisoning and gastroenteritis relentless vomiting and diarrhea rapidly deplete fluid reserves
- Fever and flu elevated body temperature accelerates fluid loss through sweating and respiration
- Heatstroke and heat exhaustion extreme temperatures and physical exertion drain fluids faster than most people can replenish them
- Severe infections pneumonia, urinary tract infections, and sepsis can cause dangerous fluid imbalances
- Chronic conditions diabetes, kidney disease, and heart conditions increase dehydration risk
- Post-surgical recovery patients unable to eat or drink normally often need IV support
- Excessive alcohol consumption alcohol is a diuretic that depletes fluids and electrolytes
- Pediatric illness young children lose proportionally more fluid during vomiting and diarrhea and are at high risk for rapid dehydration
Older adults and very young children are the most vulnerable. Both groups may not feel thirsty even when significantly dehydrated, making proactive monitoring essential.
Which IV Is Best for Hydration?
For most cases of dehydration, Normal Saline is the first-line choice. It’s effective, widely available, and safe for the vast majority of patients.
Lactated Ringer’s is considered superior in cases involving trauma, major fluid losses, or complex metabolic imbalances. Its electrolyte profile more closely mirrors human plasma, which can reduce complications when large fluid volumes are needed.
The right answer depends entirely on your clinical picture. A provider won’t just pick a fluid at random they’ll review your labs, assess your symptoms, and select the solution most likely to restore your balance safely and quickly.
What to Expect During IV Hydration at the ER
Walking into an ER when you feel terrible can be intimidating. Here’s exactly what happens when you come to ER of Irving for dehydration:
- Intake and triage A nurse assesses your symptoms and vital signs immediately. Severe cases are fast-tracked.
- Diagnostic workup On-site blood draws and urinalysis check your electrolyte levels, kidney function, and blood glucose. Results come back quickly.
- IV placement A nurse inserts a small catheter into a vein, usually in the arm. It feels like a brief pinch most patients say it’s far less uncomfortable than they expected.
- Fluid administration Your IV bag drips over 30 to 60 minutes while your vitals are monitored continuously.
- Reassessment Once the infusion is complete, the care team evaluates how you’re responding. Additional fluids or medications (like anti-nausea medicine) may be added if needed.
- Discharge instructions You’ll leave with clear guidance on fluid intake, diet, and when to return if symptoms worsen.
No long waits. No guesswork. Just fast, focused emergency care.
Why Choose ER of Irving for Dehydration Treatment?
When dehydration strikes, you want care that’s immediate, accurate, and thorough. ER of Irving is equipped to deliver all three.
Here’s what sets us apart:
- On-site diagnostics Full lab testing, X-rays, and CT scans available around the clock. We don’t send samples out and wait results come back fast so treatment starts sooner.
- Experienced emergency team Our providers are trained to manage dehydration alongside the underlying conditions driving it, whether that’s food poisoning, a cardiac event, or a pediatric emergency.
- No appointment needed Walk in any time. We’re open 24/7, including weekends and holidays.
- Comprehensive IV Fluids & Medications We carry all major IV fluid types and can add electrolytes, dextrose, anti-emetics, or pain management as clinically needed.
- Pediatric-ready We treat children with the same urgency and precision as adults, with staff experienced in recognizing dehydration in infants and toddlers.
Final Thoughts
Dehydration is easy to underestimate right up until it isn’t. The line between “I should drink more water” and “I need emergency care” can be crossed faster than most people realize, especially during illness, extreme heat, or physical exertion.
If you or someone you care for is showing signs of moderate to severe dehydration can’t keep fluids down, feels faint, has very dark urine, or seems confused don’t wait it out. Come to ER of Irving for a fast, thorough evaluation and IV treatment that works far quicker than any sports drink can.
FAQs
What fluid is best for dehydration?
Normal saline is the most commonly used IV fluid for general dehydration. Lactated Ringer’s may be preferred for trauma or more complex cases.
Which of the 4 most common IV fluids is used for hydration?
Normal Saline (0.9% NaCl) is the most frequently chosen fluid. The other three Lactated Ringer’s, Dextrose 5% in Water, and Half Normal Saline are selected based on the patient’s specific condition.
How many IV bags do you need for dehydration?
Most patients with mild to moderate dehydration need 1 bag (500–1,000 mL). Severe cases may require 2 to 3 bags, determined by the treating physician.
How long does IV hydration take at the ER?
A standard IV session lasts 30 to 60 minutes. Complex cases may take longer depending on how the patient responds.
Can you get an IV for dehydration at urgent care?
Yes, many urgent care centers offer IV hydration for moderate dehydration. For severe symptoms confusion, fainting, rapid heartbeat an emergency room is the safer choice.
Is IV hydration better than drinking water?
For severe dehydration, yes. IV fluids reach your bloodstream immediately, bypassing the digestive system. Drinking water is appropriate for mild dehydration, but it can’t keep up when the body is losing fluids rapidly.
What are the signs you need an IV for dehydration?
Key signs include inability to keep fluids down, dark urine, dizziness or fainting, confusion, sunken eyes, and a rapid heartbeat. Any of these warrants a visit to the ER.
What are the 4 main types of IV fluids?
The four main types are Normal Saline, Lactated Ringer’s, Dextrose 5% in Water (D5W), and Half Normal Saline (0.45% NaCl). Each serves a different clinical purpose and is used under medical supervision.